| Posted: Mar 16, 2015 |
Antibiotic nanoparticles attack respiratory infection
|
|
(Nanowerk News) Treating respiratory disease is often difficult because drugs have to cross biological barriers such as respiratory tissue and mucosa, and must therefore be given in large quantities in order for an effective amount to reach the target. Now researchers from Germany, Brazil and France have shown that the use of nanoparticles to carry antibiotics across biological barriers can be effective in treating lung infections. Doing so allows better delivery of the drug to the site of infection, and hence prevents the development of antibiotic resistance which may be caused by too large and continued doses of antibiotic. Additionally, such a strategy might help to overcome the rapid metabolism and excretion of the antibiotic from the body, which happens when it is administered by traditional routes, either orally or intravenously.
|
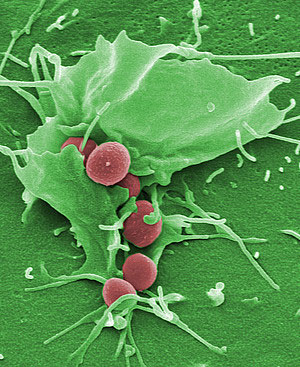 |
| The researchers used the bacterium Staphylococcus aureus as the model for their experiment which plays a crucial role in lung infections.
|
|
Describing her team’s work ("Cellular interaction and antimicrobial activity of Clarithromycin-PLGA nanocapsules") to the 13th European Respiratory Society Lung Science Conference in Estoril on the 13th of March, Dr Cristiane Carvalho-Wodarz, from the Helmholtz Institute for Pharmaceutical Research, Saarbrücken, Germany, said that, by developing nanoparticles loaded with clarithromycin, an antibiotic commonly used in the treatment of respiratory infections, they have been able to mimick the process that occurs after inhalation in vivo by delivering the drug through aerosol deposition to lung cells.
|
|
Nanoparticles, which are in the same size range as a virus - millions of times smaller than a tennis ball - were prepared by adding a biodegradable polymer oil, stabiliser and clarithromycin dissolved in solvents, to an aqueous surfactant solution. Subsequently, the solvents were completely removed. “The delivery of nanoparticles in this way enables their deposition in cells cultivated in vitro in a similar way to the deposition in vivo, which take place in the alveoli (air sacs found in the respiratory tract),” Dr Carvalho-Wodarz will say.
|
|
The researchers used the bacterium Staphylococcus aureus as the model for their experiment, since it is one of the major causes of hospital-acquired infection and also plays a crucial role in the lung infections which are common in the genetic disorder cystic fibrosis. The tiny clarithromycin nanoparticles (CLARI-NPs), were able to access the bacteria located either in biofilms (cells sticking to each other on a surface) or inside individual lung cells. “Neither of these locations is conducive to effective drug delivery through traditional routes,” says Dr Carvalho-Wodarz, “so we were pleased to see that not only did the use of CLARI-NPs allow the uptake of the antibiotic by the lung cells, but also that there were no toxic effects on all the cell types on which we tested.”
|
|
To date the work has been in vitro, using human bronchial cells. The researchers now hope to evaluate its effectiveness in an animal model, probably mice. They would also like to test the same nanoparticles loaded with other drugs used against lung infections, and in particular those in which the infectious agent becomes drug-resistant after the continued large doses that may be required.
|
|
“Using nanoparticles to deliver drugs to a local site of infection is a promising strategy for overcoming side effects, increasing treatment efficacy, and overcoming resistance. The nanoparticles we have developed have a number of advantages as drug carriers; they do not provoke a toxic effect, they are highly stable, they release the drug over a sustained period, and they can overcome cellular barriers. We believe that our formulation shows promise to improve the antibacterial efficacy which could help patients with lung infections, since the antibiotic can reach the infection site directly and therefore decrease the side effects we see during traditional routes of administration,” Dr Carvalho-Wodarz will conclude.
|

