| Posted: November 4, 2009 |
Therapeutic nanoparticles: Combating fatal brain infections |
|
(Nanowerk News) Tiny peptide particles that could be used to treat bacterial and fungal infections of the brain, such as meningitis and encephalitis, have been designed, constructed and tested successfully by researchers led by Yi-Yan Yang from the Institute of Bioengineering and Nanotechnology (IBN) of A*STAR, Singapore. The nanoparticles, which assemble themselves in water, are potent against multi-drug-resistant bacteria and can also cross the blood–brain barrier. These custom-designed nanoparticles have particular relevance to treating infections in people with suppressed immune systems, such as HIV and cancer patients, the researchers say ("Self-assembled cationic peptide nanoparticles as an efficient antimicrobial agent").
|
|
All multicellular organisms possess a variety of antimicrobial compounds known as cationic peptides. These are chains of between 12 and 50 amino acids that contain both water-interacting hydrophilic and fat-interacting hydrophobic regions. Cationic peptides can insert themselves into membranes, and are particularly attracted to negatively charged microbial membranes that they disrupt (Fig. 1), often inducing the death of the organism. Recently there has been much interest in developing these compounds as antibiotics, because they do not easily induce resistance in microbes.
|
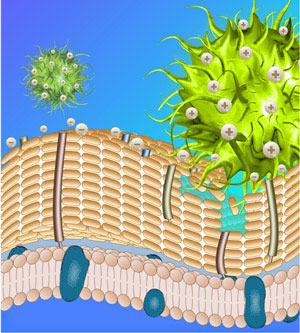 |
| Fig. 1: Schematic illustration showing how positively charged peptide nanoparticles (green) interact with and disrupt negatively charged bacterial walls.
|
|
The researchers designed their own cationic peptide from three elements—hydrophobic cholesterol, a cell-penetrating hydrophilic peptide known as TAT, and amino acids to separate them and add positive charge. In water, this compound self-assembles into tiny globular nanoparticles called micelles. Less than 200 nm in diameter, these micelles have a cholesterol core and a TAT coat.
|
|
Yang and her team at IBN determined the physical and chemical properties of their micelles and tested the antimicrobial capabilities of the nanoparticles. They found that their nanoparticles inhibited the growth of a wide variety of bacteria, fungi and yeasts; but, unlike many other antimicrobials, they did not tend to break up red blood cells.
|
|
The IBN team then collaborated with researchers at Zhejiang University in Hangzhou, China, to test the nanoparticles in living organisms. The results showed that the nanoparticles were effective against Staphylococcus aureus infections in mice, and were able to cross the blood–brain barrier to suppress bacterial growth in the brains of rabbits susceptible to meningitis. The major organs of the test animals appeared unaffected by the treatment.
|
|
“We are now planning to conduct extensive preclinical trials to evaluate the efficacy and toxicity of our nanoparticles,” says Yang. “We then look forward to progressing to clinical trials over several years.”
|

