| Aug 07, 2020 | |
Epirubicin-loaded nanomedicines beat immune checkpoint blockade resistance in glioblastoma(Nanowerk News) A nanomedicine-based strategy for chemo-immunotherapy (CIT) of glioblastoma (GBM), which has the worst prognosis among brain tumors, was successfully developed. |
|
| In vivo experiments demonstrated that the combined use of epirubicin-encapsulating nano-micelles (Epi/m) with immune checkpoint inhibitors (ICI) eradicated PTEN-negative GBM, which is highly resistant to ICI alone. Due to the synergistic effects of Epi/m plus ICI combination, the number of tumor-infiltrating T cells (TIL) and other antitumor immune cells significantly increased to kill cancer cells effectively. | |
| On the other hand, intratumoral bone marrow-derived immunosuppressive cells (MDSC), which interfere with the immune response, were significantly reduced. The CIT also provided robust immunological memory effects against the tumors, which effectively rejected newly implanted PTEN-negative GBM cells in the brain. | |
| While free epirubicin can cause damage to organs, including hematopoietic organs especially, our nanomedicine strategy significantly reduced these side effects, improving the immune response. Epi/m has already advanced into clinical trials for other cancer types, and this CIT strategy could be expected to be translated to clinical evaluation in the future. | |
| These results has been published in ACS Nano ("Translational Nanomedicine Boosts Anti-PD1 Therapy to Eradicate Orthotopic PTEN-Negative Glioblastoma"). | |
 |
|
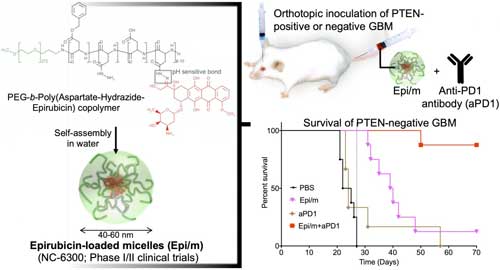
| Left: Hydrophobic epirubisin is conjugated to one end of hydrophilic polyethylene glycol (PEG) chain with aspartate-hydrazide as a linker. In water, this molecule is self-assembled to form nano-micelles (Epi/m). Upper right: PTEN(+) or PTEN(-) GBM was transplanted into the brain of mice, and Epi/m and anti-PD1 antibody (aPD1) were administered through the tail vein to evaluate survival period. Bottom right: Comparison of survival period in case of PTEN(-)GBM. PBS (phosphate buffer solution) was administered to the control group. As a result, none of the control group (black) could survive more than 30 days (8/8). Epi/m alone group (pink) died gradually after 30 days, half (4/8) in 40 days, and 7/8 by 50 days. aPD1 alone (brown) killed 6/7 within 30 days. In contrast, using Epi/m+aPD1 (red), 1/8 died 50 days later, but 7/8 were alive after 3 months even. (Image: Innovation Center of NanoMedicine) (click on image to enlarge) | |
| The Innovation Center of Nanomedicine ((Director: Prof. Kazunori Kataoka, Location: Kawasaki-City, Abbreviation: iCONM) announced that a new therapeutic option for glioblastoma (GBM) was demonstrated in mice, in a collaboration study with the Department of Bioengineering, Graduate School of Engineering, The University of Tokyo. | |
| GBM is a brain tumor with extremely rapid progression and poor prognosis (5-year survival rate: 10.1%). Although several compounds are being evaluated in clinical studies, there is no therapeutic option to significantly improve the survival period. | |
| In particular, patients with abnormalities in the PTEN gene (Note 1), one of the cancer suppressor genes, are highly resistant to currently available therapies and have high medical needs. In general, immune checkpoint inhibitors (ICIs) (Note 2) are considered to ineffective against GBM, as GBM is immunosuppressive with low T cell infiltration. | |
| In the method presented in this paper, iCONM's nano-drug delivery technology allows selective tumor accumulation of epirubicin, which causes immunogenic cell death (ICD) (Note 3), to tumor tissues, thereby, causing ICD locally for synergizing with ICI. | |
| As a result, this nanomedicine-based chemo-immunotherapy (CIT) (Note 4) was effective in mice transplanted with GBM in the brain (hereinafter referred to as mouse GBM model), and succeeded in significantly prolonging mice survival. | |
| The combination of the epirubicin-loaded nano-micelles treated mice showed high infiltration of cytotoxic T cells (TIL) (Note 5) and decreased bone marrow-derived immunosuppressive cells (MDSC) (Note 6). Eventually suppression of the immune checkpoint function was observed. | |
| Mutations in the PTEN gene occur frequently in GBM, resulting in immunosuppressive pathways that promote the resistance to ICIs. Thus, while ICIs eradicated 40% of tumors in a mouse GBM model in which the PTEN gene is normal, in a model in which the PTEN gene was knocked-out, ICIs were unable to extend mice survival. | |
| At the cellular level, it was found that PTEN-deficient cells (CT2A-luc) expressed approximately 5-fold more PDL1 than that of normal cells, which is probably connected to the therapeutic resistance with ICI. As epirubicin have shown the ability to suppress PDL1 expression in tumors, such as breast cancer (Note 7), it would be possible to decrease PDL1 levels of GBM if sufficient amount of epirubicin can be delivered into GBM lesions. | |
| Thus, CIT using nanomicelles containing epirubicin (Epi/m) in combination of ICI (Note 8) were used for enhancing the antitumor efficacy against GBM. | |
| In a GBM model with normal PTEN expression (GL261-luc), Epi/m (5 mg/kg on Epi basis) plus anti-PD1 antibodies (5 mg/kg) resulted in the survival of all mice for more than 70 days, with a remarkable extension of survival time. | |
| In this model, PBS-treated mice died within 30 days, mice treated with anti-PD1 antibodies alone (5 mg/kg) allowed 40% of mice to survive for at least 70 days, and Epi/m (5 mg/kg of Epi basis) resulted 80% of mice survival for more than 70 days. | |
| In contrast, in the PTEN-deficient model (CT2A-luc), Epi/m (5 mg/kg on Epi basis) plus anti-PD1 antibodies (5 mg/kg) resulted in only 30% of mice survival for more than 70 days, and no clear survival effect could be confirmed for the other control groups. | |
| When the dose was increased to 15 mg/kg of Epi/m (in Epi basis) and combined with anti-PD1 antibodies (5 mg/kg), 90% of mice were able to survive for more than 70 days, remarkably prolonging mice survival. | |
Notes |
|
| (Note 1) PTEN (Phosphatase and Tensin homologue deleted on chromosome 10) gene: A tumor suppressor gene that negatively regulates the PI3K/Akt signaling pathway that promotes cell proliferation. Abnormal expression of this gene, such as mutation, frequently promotes carcinogenesis and creates an environment in which disease progression easily occurs in cancer tissues. In the present study, the therapeutic effect of GMB was evaluated in both a mouse having a normal PTEN gene and a mouse having a PTEN gene knockout. | |
| (Note 2) Immune checkpoint inhibitor: When T cells infiltrating cancer tissues come close to the cancer cells, a ligand called PDL1 is expressed on the surface of the cancer cells. It is known that when PDL1 binds to the PD1 receptor on the surface of T cells, the T cells lose their role to attack cancer cells. Drugs that inhibit the binding of PDL1-PD1 are called "immune checkpoint inhibitors." In this study, mouse anti-PD1 antibody was used. | |
| (Note 3) Immune-induced cell death (ICD): Some anticancer drugs, such as epirubicin, kill cancer cells in a manner that elicits an immune response more easily than normal necrosis and apoptosis. This cell death is called immunogenic cell death, and several mechanisms have been reported, such as exposure of molecules that are targets of immune attack to the cell surface. | |
| (Note 4) Chemo-immunotherapy (CIT): A combined use of chemotherapy and immunotherapy to increase the aggressiveness of T cells that attack cancer cells, and also weaken the defense of cancer that attempts to weaken their aggressiveness to treat cancer. | |
| (Note 5) Tumor infiltrating T cells (TIL): A type of lymphocyte, T cells need to invade and contact cancer cells in order to recognize and attack specific cancer cells. In refractory cancer, there is a mechanism to prevent T cell infiltration. In order for immune checkpoint inhibitors to be effective, T cell activation is required, and for this purpose a sufficient amount of TIL is essential. | |
| (Note 6) Bone marrow-derived immunosuppressive cells (MDSC): Cancer cells secrete immunosuppressive substances and induce the production of immunosuppressive cells in the bone marrow. As a result, cells that attack cancer cells, such as T cells and dendritic cells, are inactivated, and the cancer cells can escape from immunity. For immune checkpoint inhibitors to be effective, T cell activation is required, which requires reducing the number of MDSCs. | |
| (Note 7) H. Ghebeh et al. Breast Cancer Research, 2010, 12, R48., E. M. Rom-Jurek et al. Int. J. Mol. Sci. 2018, 19. | |
| (Note 8) Nanomicelle: A spherical or rod-shaped molecular assembly with a size of several tens of nm formed by associating amphiphilic polymers with various functional molecules in water. 1 nm is one billionth of a meter. If one compares the height of a person to the diameter of the earth, the size of one cell is the size of a football stadium, and the size of a nanomicelle is the size of a soccer ball. | |
| H. Cabral, K. Miyata, K. Osada, K. Kataoka, "Block copolymer micelles in nanomedicine applications" Chem. Rev. 2018, 118 6844-6892. (DOI: 10.1021/acs.chemrev.8b00199) |
| Source: Innovation Center of NanoMedicine | |
|
Subscribe to a free copy of one of our daily Nanowerk Newsletter Email Digests with a compilation of all of the day's news. |
