| Posted: April 26, 2007 |
Organ printing |
|
(Nanowerk News) The dearth of transplantable organs, as well as cultural taboos on organ donation and transplant acceptance, could have a solution in the future if the promise of tissue engineering can be fulfilled. The vision is simply this: rather than harvest organs, let's build them from scratch ( "Bioprinting living structures").
|
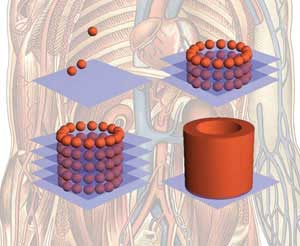 |
| Bio-ink droplets are printed onto biopaper to build elaborate 3D networks of cells. (Image: Chemical Biology)
|
|
In order to build an organ, you need four components: cells (the bio-ink), a biomaterial (the biopaper), a device to make three-dimensional structures (the bioprinter), and a method to aid tissue assembly and maturation (the bioreactor). In addition to this shopping list, you need the expertise to put the components together, and you need funding. Enter the hydrogel chemists, the cell and developmental biologists, the physicists, the computational modellers, and a company that builds rapid prototyping devices. With funding from the highly competitive US National Science Foundation's Frontiers in Integrative Biological Research (FIBR) program, our multidisciplinary team, led by Gabor Forgacs at the University of Missouri in Columbia, US, is attempting to harness biology to build organs from cells.
|
|
Tissue engineering, which integrates biomaterials with cell and developmental biology, is an applied science with the goal of generating implantable tissues and organ structures to improve human health. As an engineering discipline, its practitioners have an obligation to build systems with customer-dictated design criteria in mind. To arrive at a useful product, tissue engineers must understand what physicians and patients actually want and what insurance companies will reimburse. This end-user focus dictates that to achieve complexity, we must focus on simplicity.
|
|
Current cell therapies are limited, aside from cell sourcing issues, by three scientific problems: cell delivery, cell retention, and cell integration. What is needed is a biomaterial that will provide the relevant sequence of signals for cell expansion, differentiation, and self-organisation into a tissue. This biomaterial should be printable in three dimensions, and also allow biology and the physics of liquids to do the 'heavy lifting' of creating a complex tissue from aggregated cells. Cells must be able to remodel the biomaterial scaffolding into a natural extracellular matrix. Materials from the 20th century - for example, polyethylene meshes and Teflon - will not work; 21st century materials are bio-inspired and mimic both the composition and mechanical properties of the extracellular matrix. To this end, we developed a covalently cross-linked, biodegradable mimic of the extracellular matrix that supports 3D cell cultures in vitro and allows functional tissues to grow in vivo.
|
|
Yet, in many ways, the biomaterial is the easy part. Shaping an artificial 'neo-organ', developing the printing tools and a computer model for layer-by-layer construction, and devising a strategy to mature the neo-organ before transplantation are among the main challenges.
|
|
The basic principle employed by the FIBR team is self-assembly, a fundamental process that drives organisation in living and non-living systems. Important to organ printing is the seminal observation that, while developmental patterning during embryogenesis is under strict genetic control, it is the underlying physical principles that allow complex structures to form.
|
|
Organised networks of tubes are an essential feature of most organs in our bodies. Such networks control and regulate the macroscopic and microscopic properties of the organs. Our vascular and lymphatic systems, our bones, our gastrointestinal and reproductive organs, and even our liver and kidneys are elaborately interconnected tubes. Our team uses bioprinting to manipulate aggregates of cells into branched networks of tubular structures. We have analysed heart-valve and limb genesis during chick development, and have used these basic principles to model and replicate cellular self-assembly. In future work, branched vascular trees will be printed with progressively reduced internal diameters, and bioreactors optimised for vascular maturation. While the fulfilment of the tissue engineering vision may still be years away, the near future could see the four components of bioprinting deliver ex vivo human organoids for use in the discovery and toxicological evaluation of new pharmaceuticals.
|

