| Posted: Jun 13, 2012 | |
Medical textiles: Nanofiber-based 'smart' dressings for burn wounds |
|
| (Nanowerk Spotlight) Burn injuries are one of the major global health problems. As per a recent report of World Health Organization (WHO), every year 195,000 people from all over the world die because of fire alone. Additionally, most of the people who survive from burn injuries carry the stigma for lifetime disabilities and deformity. Over 95% of burn-related deaths have been accounted from low-income countries as most of the high-income countries have made major advances in fire-prevention strategies and burn care. South-East Asia is on the top for fire-related deaths and also for the burn mortality rate among women1. | |
| A burn injury may damage some or all skin layers and is caused by a hot solid, a hot liquid (scalding) or a flame (Source: International Society for Burn Injuries (ISBI)). However, injuries related to electricity, radioactivity, ultraviolet radiation, chemicals and respiratory damage due to smoking are also considered as burn injuries. There are various systems for classifying burn wounds such as: | |
| By severity: As per this system, burn injuries can be major, moderate or minor (American Burn Association) based on various factors like patient's age, total body surface area (TBSA) burnt and co-morbidities. | |
| By Surface area: The "Rules of Nines" is applied to determine the burnt area where burnt body is divided into sections and each section is equal to 9% of TBSA. | |
| By depth: Ambroise Pare, a French barber-surgeon devised this system of classification which is based on the depth of a burn injury. As per this system burns can be divided into first, second and third/fourth degrees. | |
| Apart from breathing, pain, nutritional and circulatory maintenance, it is extremely important to protect a burn wound from microbial infections because of low levels of cell mediated immunity and skin injury. These infections are mostly caused by fungi and bacteria like methicillin-resistant Staphylococcus aureus (MRSA) and Pseudomonas aeruginosa, which release various proteases, adhesion and colonization proteins that damage adherent tissues2, 3. | |
| Besides cleaning the wound and applying various topical anti-microbial agents, wound dressings could be an effective solution in preventing microbial infections for burn care4. The suitability of a burn wound dressing depends on a burn type. Conventional dressings are not efficient enough to induce haemostasis (mechanism to stop bleeding), adherence and in holding a moist environment around wound5. Due to the advances in the field of nanotechnology, it is now possible to design nanofiber-based wound dressings (NFDs) where an electrospun-nanofibrous layer is applied to a basic support fabric material. NFDs have the following advantages6,7: | |
|
|
|
| Additionally, NFDs operate in moist environment, do not require frequent changing and thus reduce pain and scars which is extremely beneficial for burn victims. | |
 |
|
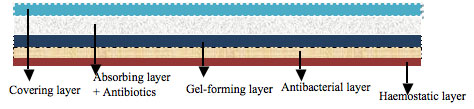
| Multi-layering capacity of nanofiber-based wound dressings. | |
| Nanofibers are prepared by a series of techniques; however, electrospinning is mostly used to synthesize polymeric nanofibers8. Additionally, protein nanofibers (tropoelastin) have also been shown to have immense potential in making NFDs9. | |
| HemCon Med. Tech. Inc. (http://www.hemcon.com), Smith & Nephew (http://wound.smith-nephew.com), Covidien (www.covidien.com) and Integra Life Sciences (http://www.integralife.com) are some of the major companies engaged in the commercial production of NFDs. Elmarco (http://www.elmarco.cz) is developing a series of wound-care products with the help of their patented Nanospider™ technology in collaboration with Alltracel/HemCon (http://www.hemcon.com) which uses m.doc™ technology to develop haemostatic NFDs. Other patented technologies for the commercial manufacturing of nanofibers include Nanoval™ by Nanoval Gmbh & Co. (http://www.nanoval.de), Hills Melt Blown Technology™ by Hills Inc. (http://www.hillsinc.net) and Platform Technology™ by Nanotope (http://www.nanotope.com). Some key NFD products are given in Table 1. | |
 |
|
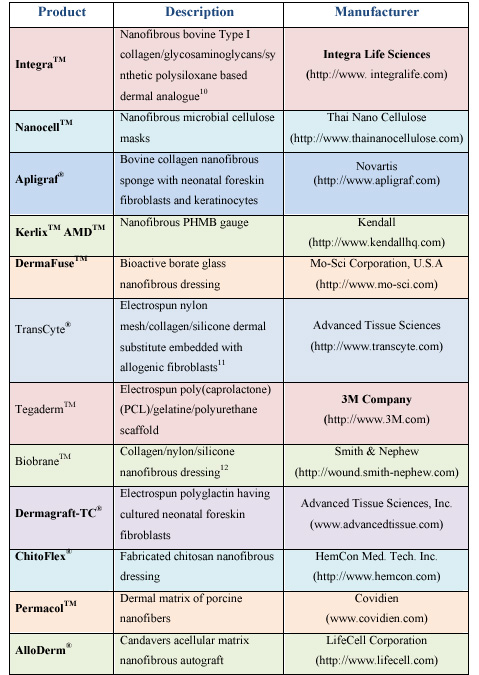
| Table 1: Key nanofiber-based burn wound-care products. | |
| In 2010, the global advanced wound care market was around $6.2 billion13 and is estimated to grow up to 12% in the coming few years. As per worldwide statistics, for burn wound care, a startling amount of $5 billion is required annually. These statistics demonstrate a potential market for burn care products and need for cost-effective dermal rehabilitation to make it available to general public. As NFDs are more efficient and less traumatic, it is expected that they would capture a significant amount of advanced wound care market share in the future. Recent breakthroughs and R&D activities in the field of NFDs are as follows: | |
| Chitosan-coated poly(vinyl alcohol) nanofibers for wound dressings7: | |
| Heat-treated PVA nanofibrous matrix coated with chitosan solution to construct a biomimetic NFD. The mechanical stability and histological studies showed that this dressing was a better accelerator for wound healing, less hydrophilic and more tensile. | |
| Hyperbranched polyglycerol(HPGL) NFD as drug delivery vehicle14: | |
| A nanofibrous dressing of HPGL having Calendula officinalis which is an anti-inflammatory and wound healing agent was prepared and studies showed that HPGL nanofibers could prove to have drug delivery properties when used as NFD for wound care. | |
| SiO2 NFD with embedded silver nanoparticles as recoverable wound cover15: | |
| Silver nanoparticles (Ag NPs) were embedded on SiO2 nanofibers and results showed that due to the conformability of SiO2 nanofibers, this dressing facilitated convenient patterning into a shape required for wound cover. Embedded Ag NPs showed a long-term antibacterial effect while inorganic part of this NFD could be recovered through calcinations without lost of any flexibility. | |
| Degradability of collagen could be improved by combining it with zein16: | |
| Addition of zein could improve the electrospinnability of collagen while various other mechanical and in vitro degradable properties of the dressing could be regulated by altering collagen/zein blending ratio. | |
| Nano ZnO in combination with Sodium alginate/poly(vinyl alcohol) nanofibers to enhance antibacterial property17: | |
| Presence of nano-ZnO could improve antibacterial properties of sodium alginate/PVA nano-mats especially over Escherichia coli and Staphylococcus aureus; however, optimal concentration of ZnO is yet to be formulated for providing maximum antibacterial activity with least toxicity is yet to be identified. | |
| Regulated release of dual drugs with composite nanofibers containing drug-loaded nanoparticles18: | |
| By adjusting the preparation process of the electrospinning solution, programmable release of dual drugs could be achieved through NFDs. This technique might be an effective way for an early wound healing. | |
| Challenges and Future Prospects | |
| Although modern-age NFDs are more effective than conventional dressings, they are very expensive. NFDs are extremely difficult to handle due to their delicacy and require some kind of tangible support; however, chemical properties of the support fabric make nanofiber coating heterogeneous19. In addition, nanofibers often show poor adhesion to the base support. In a recent study20, plasma-treated cotton gauzes were used as the support fabric after electrospinning chitosan nanofibers, where nanofibers showed better adhesion, a low rate of degradation and moisture vapour transport. | |
| Thus a special care has to be taken in choosing a suitable combination of nanofiber and support fabric for making NFDs; however, with the recent nanotechnological advancements, we can expect many more efficient NFD products in the future. | |
| References | |
| 1. Violence and Injury Prevention | |
| 2. Ma Kun, "Biomimetic nanofiber/stem cell composite for skin graft application", (2009), NUS | |
| 3. Microbial Infection of Burn Wounds | |
| 4. Victor T. Tchemtchoua et al., "Development of a Chitosan Nanofibrillar Scaffold for Skin Repair and Regeneration", Biomacromolecules, ACS, 12 (9), (2011) 3194-3204 | |
| 5. Alves Janete Lara, Bellino Nuno JosÉ, Geraldes Maria José, "Nano-Bioabsorbent Composite Wound Dressing for Exudate Management", John Wiley & Sons, Inc., WIREs Nanomed Nanobiotechnology, (2010) 510-525 | |
| 6. Zahedi et al., "A review on wound dressings with an emphasis on electrospun nanofibrous polymeric bandages", John Wiley & Sons, Ltd., Polym. Adv. Technol., 21, (2010) 77-95 | |
| 7. Kang YO et al., "Chitosan-coated poly (vinyl alcohol) nanofibers for wound dressings", J. Biomed. Mater. Res. B. Appl. Biomater, 92 (2), (2010) 568-76 | |
| 8. S Sell et al., "Extracellular matrix regenerated: tissue engineering via electrospun biomimetic nanofibers", Society of Chemical Industry, Polym. Int., 56, (2007) 0959-8103 | |
| 9. Li et al., "Electrospun protein fibers as matrices for tissue engineering", Biomaterials, 26, (2005) 5999-6008 | |
| 10. Chong Ee Jay, "Nanofibrous Mat for Tissue Engineering, Wound Dressing and Dermal Reconstitution", (2006), NUS | |
| 11. S. P. Zhong, Y. Z. Zhang, C. T. Lim, "Tissue scaffolds for skin wound healing and dermal reconstruction", John Wiley & Sons, Inc., WIREs Nanomed Nanobiotechnology, 2, (2010) 510-525 | |
| 12. Wound Care | |
| 13. http://www.visiongain.com Advanced Wound Care World Market Prospects 2011-2021 | |
| 14. Vargas EA et al., "Hyperbranched polyglycerol electrospun nanofibers for wound dressing applications", Acta Biomater, 6 (3), (2010) 1069-78 | |
| 15. Zhijun Ma et al., "Silver nanoparticles decorated flexible SiO2 nanofibers with long-term antibacterial effect as reusable wound cover", Colloids and Surfaces A: Physicochem. Eng. Aspects, 387, (2011) 57-64 | |
| 16. Jiantao Lin et al., "Co-electrospun Nanofibrous Membranes of Collagen and Zein for Wound Healing", ACS Applied Materials & Interfaces, Article ASAP (2012) | |
| 17. Shalumon KT et al., "Sodium alginate/poly (vinyl alcohol)/nano ZnO composite nanofibers for antibacterial wound dressings", Int. J. Biol. Macromol., 49 (3), (2011) 247-54 | |
| 18. Yazhou Wang et al., "Electrospun composite nanofibers containing nanoparticles for the programmable release of dual drugs", Polymer Journal, NPG, 43, (2011) 478-483 | |
| 19. Challenges in Advanced Nanofiber Wound Dressings Annual Report, NTC Project, (2009) | |
| 20. Marian McCord, "Challenges in Advanced Nanofiber Wound Dressings, Annual Report, October 2010", NTC Project: F09-NS06 | |
| By - Abhilasha Varma, Centre for Knowledge Management of Nanoscience & Technology (CKMNT), Email: [email protected] | |
|
Become a Spotlight guest author! Join our large and growing group of guest contributors. Have you just published a scientific paper or have other exciting developments to share with the nanotechnology community? Here is how to publish on nanowerk.com. |
|
