Showing Spotlights 321 - 328 of 544 in category All (newest first):
 MicroRNAs (miRNAs) are short ribonucleic acid molecules, consisting of 21-25 nucleotide bases, that negatively regulate gene expression, also termed as gene silencing. Each miRNA is thought to regulate multiple genes, and since the human genome encodes hundreds of miRNAs, the potential regulatory circuitry afforded by miRNA is enormous. Recent discoveries suggest the association of specific miRNA sequences with a spectrum of diseases including cardiovascular and autoimmune diseases, as well as with a variety of cancers. It is therefore imperative, for diagnostics and prognostics, to accurately measure the expression levels of target miRNA molecules in patients' tissue samples or body fluids. To that end, researchers have developed an alternative way for the direct analysis of miRNAs in an array format, demonstrating fast and ultrasensitive detection of specific miRNAs.
MicroRNAs (miRNAs) are short ribonucleic acid molecules, consisting of 21-25 nucleotide bases, that negatively regulate gene expression, also termed as gene silencing. Each miRNA is thought to regulate multiple genes, and since the human genome encodes hundreds of miRNAs, the potential regulatory circuitry afforded by miRNA is enormous. Recent discoveries suggest the association of specific miRNA sequences with a spectrum of diseases including cardiovascular and autoimmune diseases, as well as with a variety of cancers. It is therefore imperative, for diagnostics and prognostics, to accurately measure the expression levels of target miRNA molecules in patients' tissue samples or body fluids. To that end, researchers have developed an alternative way for the direct analysis of miRNAs in an array format, demonstrating fast and ultrasensitive detection of specific miRNAs.
Jun 6th, 2011
 It is widely believed that stem cell therapies have the potential to revolutionize the treatment of human diseases. Key to the success of such therapies are two crucial properties: the ability of stem cells to develop into any specialized cell type depending on the specific need at hand; and the ability to guide the fate of the stem cells by various external factors. Researchers in Asia have now demonstrated that graphene provides a promising biocompatible scaffold that does not hamper the proliferation of human mesenchymal stem cells and accelerates their specific differentiation into bone cells. The differentiation rate is comparable to the one achieved with common growth factors, demonstrating graphene's potential for stem cell research.
It is widely believed that stem cell therapies have the potential to revolutionize the treatment of human diseases. Key to the success of such therapies are two crucial properties: the ability of stem cells to develop into any specialized cell type depending on the specific need at hand; and the ability to guide the fate of the stem cells by various external factors. Researchers in Asia have now demonstrated that graphene provides a promising biocompatible scaffold that does not hamper the proliferation of human mesenchymal stem cells and accelerates their specific differentiation into bone cells. The differentiation rate is comparable to the one achieved with common growth factors, demonstrating graphene's potential for stem cell research.
May 24th, 2011
 Superparamagnetic iron oxide nanoparticles (SPIONs) are emerging as promising candidates for various biomedical applications such as enhanced resolution imaging or targeted drug or gene delivery due to their biocompatibility, low cost of production, ability to immobilize biological materials on their surfaces, and potential for direct targeting using external magnets. Over the past few years, researchers demonstrated that magnetofection is an appropriate tool for rapid and specific gene transfection with low dose in vitro and site-specific in vivo applications. In new work, scientists in Australia have now successfully demonstrated the use of magnetofection for the delivery of malaria DNA vaccine.
Superparamagnetic iron oxide nanoparticles (SPIONs) are emerging as promising candidates for various biomedical applications such as enhanced resolution imaging or targeted drug or gene delivery due to their biocompatibility, low cost of production, ability to immobilize biological materials on their surfaces, and potential for direct targeting using external magnets. Over the past few years, researchers demonstrated that magnetofection is an appropriate tool for rapid and specific gene transfection with low dose in vitro and site-specific in vivo applications. In new work, scientists in Australia have now successfully demonstrated the use of magnetofection for the delivery of malaria DNA vaccine.
May 11th, 2011
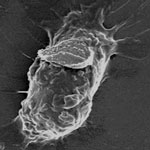 Macrophages are white blood cells with a wide presence in various organs and tissues, that perform an essential role in keeping organisms healthy by scavenging cellular debris and disease agents. Since macrophages play an indispensable role in most pathological conditions, they represent an ideal target for therapeutic applications. Several approaches seeking to use macrophages for targeted therapies involve feeding therapeutic nanoparticles to macrophages ex vivo, followed by re-injection of the macrophages to target the diseased site. These techniques are often hampered by reduced drug release rates and drug degradation. Overcoming these limitations, scientists now report the ability of cellular backpacks to successfully encapsulate and controllably release drugs and avoid phagocytic internalization while remaining on the macrophage's surface.
Macrophages are white blood cells with a wide presence in various organs and tissues, that perform an essential role in keeping organisms healthy by scavenging cellular debris and disease agents. Since macrophages play an indispensable role in most pathological conditions, they represent an ideal target for therapeutic applications. Several approaches seeking to use macrophages for targeted therapies involve feeding therapeutic nanoparticles to macrophages ex vivo, followed by re-injection of the macrophages to target the diseased site. These techniques are often hampered by reduced drug release rates and drug degradation. Overcoming these limitations, scientists now report the ability of cellular backpacks to successfully encapsulate and controllably release drugs and avoid phagocytic internalization while remaining on the macrophage's surface.
May 10th, 2011
 The potential use of antimicrobial surface coatings ranges from medicine, where medical device infection is associated with significant healthcare costs, to the construction industry and the food packaging industry. Thin films containing silver nanoparticles have been seen as promising candidate coatings. Silver is known as one of the oldest antimicrobial agents. Silver ions are thought to inhibit bacterial enzymes and bind to DNA. Silver nanomaterials have been used effectively against different bacteria, fungi and viruses. Using something like an advanced form of a rubber stamp, scientists have now developed a way to adhere an ultra-thin (just a few molecules thick) antibacterial coating to a wound. The "stamped" area shows bactericidal activity for at least 48 hours.
The potential use of antimicrobial surface coatings ranges from medicine, where medical device infection is associated with significant healthcare costs, to the construction industry and the food packaging industry. Thin films containing silver nanoparticles have been seen as promising candidate coatings. Silver is known as one of the oldest antimicrobial agents. Silver ions are thought to inhibit bacterial enzymes and bind to DNA. Silver nanomaterials have been used effectively against different bacteria, fungi and viruses. Using something like an advanced form of a rubber stamp, scientists have now developed a way to adhere an ultra-thin (just a few molecules thick) antibacterial coating to a wound. The "stamped" area shows bactericidal activity for at least 48 hours.
May 5th, 2011
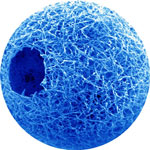 Damaged articular cartilages, like the ones found in the knee joint, ordinarily demonstrate a very limited capability for self-healing. Functional restoration of diseased or damaged articular cartilage is a major clinical challenge. There have been a number of successful approaches to tissue engineered cartilage, including the use of natural and synthetic biomaterial scaffolds. Although recent progress has been made in engineering cartilage of various shapes and sizes for cosmetic purposes, current treatments for cartilage repair are less than satisfactory, and rarely restore full function or return the tissue to its native state. Researchers have now developed nanofibrous hollow microspheres self-assembled from star-shaped biodegradable polymers as an injectable cell carrier. When the spheres are injected with cells into wounds, these spheres biodegrade, but the cells live on to form new tissue.
Damaged articular cartilages, like the ones found in the knee joint, ordinarily demonstrate a very limited capability for self-healing. Functional restoration of diseased or damaged articular cartilage is a major clinical challenge. There have been a number of successful approaches to tissue engineered cartilage, including the use of natural and synthetic biomaterial scaffolds. Although recent progress has been made in engineering cartilage of various shapes and sizes for cosmetic purposes, current treatments for cartilage repair are less than satisfactory, and rarely restore full function or return the tissue to its native state. Researchers have now developed nanofibrous hollow microspheres self-assembled from star-shaped biodegradable polymers as an injectable cell carrier. When the spheres are injected with cells into wounds, these spheres biodegrade, but the cells live on to form new tissue.
May 4th, 2011
 Heparin is widely used as an anti-coagulant to prevent the formation of blood clots. This naturally occurring biological molecule is commonly used during surgery for blood thinning. At the end of surgery, heparin has to be removed in order to allow the blood to clot again - this is currently done using a protein called protamine, the only clinically approved heparin binder. Unfortunately, protamine can cause severe allergic reactions in a number of patients. Researchers at the University of York have now developed a synthetic molecule which is capable of binding heparin just as effectively as protamine. The team's approach may eventually be useful for developing protamine replacements.
Heparin is widely used as an anti-coagulant to prevent the formation of blood clots. This naturally occurring biological molecule is commonly used during surgery for blood thinning. At the end of surgery, heparin has to be removed in order to allow the blood to clot again - this is currently done using a protein called protamine, the only clinically approved heparin binder. Unfortunately, protamine can cause severe allergic reactions in a number of patients. Researchers at the University of York have now developed a synthetic molecule which is capable of binding heparin just as effectively as protamine. The team's approach may eventually be useful for developing protamine replacements.
May 2nd, 2011
 A few years ago, researchers determined that the stiffness of cancer cells affects the way they spread. When cancer is becoming metastatic, or invading other organs, the diseased cells must travel throughout the body. Because the cells need to enter the bloodstream and maneuver through tight anatomical spaces, cancer cells are much more flexible, or softer, than normal cells. With this knowledge, researchers wanted to understand the cell mechanics associated with the anticancer treatment of cells from patient samples; in particular they were interested in reporting the effects of green tea extract due to the fact that is was a natural product, it has know anti-cancer effects and it is widely consumed in beverage form around the world.
A few years ago, researchers determined that the stiffness of cancer cells affects the way they spread. When cancer is becoming metastatic, or invading other organs, the diseased cells must travel throughout the body. Because the cells need to enter the bloodstream and maneuver through tight anatomical spaces, cancer cells are much more flexible, or softer, than normal cells. With this knowledge, researchers wanted to understand the cell mechanics associated with the anticancer treatment of cells from patient samples; in particular they were interested in reporting the effects of green tea extract due to the fact that is was a natural product, it has know anti-cancer effects and it is widely consumed in beverage form around the world.
Apr 5th, 2011
 MicroRNAs (miRNAs) are short ribonucleic acid molecules, consisting of 21-25 nucleotide bases, that negatively regulate gene expression, also termed as gene silencing. Each miRNA is thought to regulate multiple genes, and since the human genome encodes hundreds of miRNAs, the potential regulatory circuitry afforded by miRNA is enormous. Recent discoveries suggest the association of specific miRNA sequences with a spectrum of diseases including cardiovascular and autoimmune diseases, as well as with a variety of cancers. It is therefore imperative, for diagnostics and prognostics, to accurately measure the expression levels of target miRNA molecules in patients' tissue samples or body fluids. To that end, researchers have developed an alternative way for the direct analysis of miRNAs in an array format, demonstrating fast and ultrasensitive detection of specific miRNAs.
MicroRNAs (miRNAs) are short ribonucleic acid molecules, consisting of 21-25 nucleotide bases, that negatively regulate gene expression, also termed as gene silencing. Each miRNA is thought to regulate multiple genes, and since the human genome encodes hundreds of miRNAs, the potential regulatory circuitry afforded by miRNA is enormous. Recent discoveries suggest the association of specific miRNA sequences with a spectrum of diseases including cardiovascular and autoimmune diseases, as well as with a variety of cancers. It is therefore imperative, for diagnostics and prognostics, to accurately measure the expression levels of target miRNA molecules in patients' tissue samples or body fluids. To that end, researchers have developed an alternative way for the direct analysis of miRNAs in an array format, demonstrating fast and ultrasensitive detection of specific miRNAs.
 Subscribe to our Nanotechnology Spotlight feed
Subscribe to our Nanotechnology Spotlight feed





