Showing Spotlights 337 - 344 of 544 in category All (newest first):
 Imagine intelligent medical implants that can continuously monitor their condition inside the body and autonomously respond to changes such as infection by releasing anti-inflammatory agents. Thanks to nanotechnology, medical research is moving quickly towards this goal. A new study shows that the use of polypyrrole films as electrically controlled drug release devices on implant surfaces can potentially improve bone implants. By electrodepositing antibiotics or anti-inflammatory drugs in a polymer coating on medical devices, researchers demonstrate that such drugs can be released from polypyrrole on demand - by applying a voltage - and control cellular behavior important for orthopedic applications, i.e. inhibit inflammation and kill bacteria.
Imagine intelligent medical implants that can continuously monitor their condition inside the body and autonomously respond to changes such as infection by releasing anti-inflammatory agents. Thanks to nanotechnology, medical research is moving quickly towards this goal. A new study shows that the use of polypyrrole films as electrically controlled drug release devices on implant surfaces can potentially improve bone implants. By electrodepositing antibiotics or anti-inflammatory drugs in a polymer coating on medical devices, researchers demonstrate that such drugs can be released from polypyrrole on demand - by applying a voltage - and control cellular behavior important for orthopedic applications, i.e. inhibit inflammation and kill bacteria.
Jan 25th, 2011
 Chemotherapeutics generally show a delicate balance between maintaining a high enough dose to kill cancer cells while avoiding a dose so high that it causes severe toxic effects. One of the many promises of nanomedicine is a class of nanoscale drug delivery vehicles that can pinpoint cancer cells and deliver their tumor-killing payload right into cancer cells with high efficiency and no side effects. Based on a novel silica 'nanorattle' structure, a research team further extended their work to fabricate 'all-in-one' multifunctional gold nanoshells on silica nanorattles which combine remote-controlled photothermal therapy with chemotherapy. The results indicate that a combination of hyperthermia and chemotherapeutic agents is an encouraging approach to optimizing cancer therapy for the synergistic effects are greater than the two individual treatments alone.
Chemotherapeutics generally show a delicate balance between maintaining a high enough dose to kill cancer cells while avoiding a dose so high that it causes severe toxic effects. One of the many promises of nanomedicine is a class of nanoscale drug delivery vehicles that can pinpoint cancer cells and deliver their tumor-killing payload right into cancer cells with high efficiency and no side effects. Based on a novel silica 'nanorattle' structure, a research team further extended their work to fabricate 'all-in-one' multifunctional gold nanoshells on silica nanorattles which combine remote-controlled photothermal therapy with chemotherapy. The results indicate that a combination of hyperthermia and chemotherapeutic agents is an encouraging approach to optimizing cancer therapy for the synergistic effects are greater than the two individual treatments alone.
Jan 17th, 2011
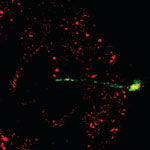 With the advance of nanomedicine, bio-nanotechnology, and molecular biology, researchers require tools that allow them to work on a single cell level. These tools are required to probe individual cells, monitor their processes, and control/alter their functions through nanosurgery procedures and injection of drugs, DNA etc. - all without damaging the cells, of course. Researchers have now developed a multifunctional endoscope-like device, using individual CNTs for prolonged intracellular probing at the single-organelle level, without any recordable disturbance to the metabolism of the cell. These endoscopes can transport attoliter volumes of fluid, record picoampere signals from cells, and can be manipulated magnetically. Furthermore, the tip deflects with submicrometer resolution, and the attachment of gold nanoparticles allows intracellular fingerprinting using surface-enhanced Raman spectroscopy (SERS).
With the advance of nanomedicine, bio-nanotechnology, and molecular biology, researchers require tools that allow them to work on a single cell level. These tools are required to probe individual cells, monitor their processes, and control/alter their functions through nanosurgery procedures and injection of drugs, DNA etc. - all without damaging the cells, of course. Researchers have now developed a multifunctional endoscope-like device, using individual CNTs for prolonged intracellular probing at the single-organelle level, without any recordable disturbance to the metabolism of the cell. These endoscopes can transport attoliter volumes of fluid, record picoampere signals from cells, and can be manipulated magnetically. Furthermore, the tip deflects with submicrometer resolution, and the attachment of gold nanoparticles allows intracellular fingerprinting using surface-enhanced Raman spectroscopy (SERS).
Dec 15th, 2010
 The use of minute particles as drug carriers for targeted therapy has been studied and discussed for more than 20 years. A selective accumulation of active substances in target tissues has been demonstrated for certain so-called nanocarrier systems that are administered bound to pharmaceutical drugs. Great expectations are placed on nanocarrier systems that can overcome natural barriers such as the blood-brain barrier (BBB) and transport the medication directly to the desired tissue and thus heal neurological diseases that were formerly incurable. The BBB represents the border between the circulating blood and the fluid in the central nervous system. It functions to protect the sensitive nerve cells from foreign substances and infections from the blood. Whether nanoparticles enter the central nervous system unintentionally and induce health problems is also being debated.
The use of minute particles as drug carriers for targeted therapy has been studied and discussed for more than 20 years. A selective accumulation of active substances in target tissues has been demonstrated for certain so-called nanocarrier systems that are administered bound to pharmaceutical drugs. Great expectations are placed on nanocarrier systems that can overcome natural barriers such as the blood-brain barrier (BBB) and transport the medication directly to the desired tissue and thus heal neurological diseases that were formerly incurable. The BBB represents the border between the circulating blood and the fluid in the central nervous system. It functions to protect the sensitive nerve cells from foreign substances and infections from the blood. Whether nanoparticles enter the central nervous system unintentionally and induce health problems is also being debated.
Dec 8th, 2010
 Silica nanomaterials have shown great promise for delivering anticancer and other water-insoluble drugs into human cancer cells. The high surface area, tunable pore diameter, and uniform mesoporous structure of the mesoporous silicas offer a unique advantage for loading and releasing large quantities of biomedical agents. These properties are beneficial for designing stimuli-response drug release and allow mesoporous silica nanoparticles (MSN) to be loaded with a drug. Especially MSNs with hollow and rattle structure show particularly higher drug loading efficiency because the interstitial hollow space can selectively and efficiently accommodate drug molecules. In what represents a significant progress of in vivo cancer therapy with mesoporous silica nanomaterials, researchers have demonstrated that silica nanorattles show advantages for in vivo enhancement of therapy efficacy and reducing the systematic toxicity of antitumor drugs.
Silica nanomaterials have shown great promise for delivering anticancer and other water-insoluble drugs into human cancer cells. The high surface area, tunable pore diameter, and uniform mesoporous structure of the mesoporous silicas offer a unique advantage for loading and releasing large quantities of biomedical agents. These properties are beneficial for designing stimuli-response drug release and allow mesoporous silica nanoparticles (MSN) to be loaded with a drug. Especially MSNs with hollow and rattle structure show particularly higher drug loading efficiency because the interstitial hollow space can selectively and efficiently accommodate drug molecules. In what represents a significant progress of in vivo cancer therapy with mesoporous silica nanomaterials, researchers have demonstrated that silica nanorattles show advantages for in vivo enhancement of therapy efficacy and reducing the systematic toxicity of antitumor drugs.
Dec 7th, 2010
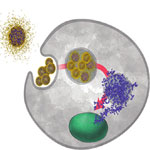 Scientists have shown that two pH response moieties - a pH solubility switch and a pH labile group - can be incorporated into the backbone of polymers which can then be formulated into dual responsive nanoparticles encapsulating small hydrophobic molecules and larger protein payloads. As nanoparticles they function akin to an AND logic gate. The beta-aminoester backbone moiety provides a pH triggered solubility switch, only when this switch is 'ON' does the ketal moiety also turn 'ON' to undergo rapid acid catalyzed hydrolysis. This system seems to be a promising vehicle for the administration of hydrophilic and hydrophobic payloads into target areas of the human body.
Scientists have shown that two pH response moieties - a pH solubility switch and a pH labile group - can be incorporated into the backbone of polymers which can then be formulated into dual responsive nanoparticles encapsulating small hydrophobic molecules and larger protein payloads. As nanoparticles they function akin to an AND logic gate. The beta-aminoester backbone moiety provides a pH triggered solubility switch, only when this switch is 'ON' does the ketal moiety also turn 'ON' to undergo rapid acid catalyzed hydrolysis. This system seems to be a promising vehicle for the administration of hydrophilic and hydrophobic payloads into target areas of the human body.
Nov 24th, 2010
 A multi-disciplinary research team has introduced a novel label-free optofluidic-nanoplasmonic biosensor and demonstrated direct detection of live viruses from biological media at medically relevant concentrations with little to no sample preparation. This novel platform can be easily adapted for point-of-care diagnostics to detect a broad range of viral pathogens in resource-limited clinical settings at the far corners of the world, in defense and homeland security applications as well as in civilian settings such as airports or other public spaces. This work is the first demonstration of detection of intact viruses using extraordinary light transmission phenomena in plasmonic nanohole arrays.
A multi-disciplinary research team has introduced a novel label-free optofluidic-nanoplasmonic biosensor and demonstrated direct detection of live viruses from biological media at medically relevant concentrations with little to no sample preparation. This novel platform can be easily adapted for point-of-care diagnostics to detect a broad range of viral pathogens in resource-limited clinical settings at the far corners of the world, in defense and homeland security applications as well as in civilian settings such as airports or other public spaces. This work is the first demonstration of detection of intact viruses using extraordinary light transmission phenomena in plasmonic nanohole arrays.
Nov 17th, 2010
 Medical researchers believe that the best way to protect eye from glaucoma is to protect the optic nerve from a sudden increase in intraocular pressure since ocular hypertension is the most important risk factor for glaucoma. Accordingly, for the past few years, huge research efforts have been made to develop a powerful biotechnical approach to protect the optic nerve. As a result, scientists discovered that Heat Shock Proteins (HSPs) can be a new powerful modality for the protection of optic nerves - ocular neuroprotection - from glaucoma. Although a variety of methods to induce HSPs have been developed and tried, they all were found to be ineffective for the induction of HSPs from the optic nerve due to side effects including chemical and physical side effects. A novel nanomedicine modality has now been shown to be feasible for ocular neuroprotection in glaucoma cases.
Medical researchers believe that the best way to protect eye from glaucoma is to protect the optic nerve from a sudden increase in intraocular pressure since ocular hypertension is the most important risk factor for glaucoma. Accordingly, for the past few years, huge research efforts have been made to develop a powerful biotechnical approach to protect the optic nerve. As a result, scientists discovered that Heat Shock Proteins (HSPs) can be a new powerful modality for the protection of optic nerves - ocular neuroprotection - from glaucoma. Although a variety of methods to induce HSPs have been developed and tried, they all were found to be ineffective for the induction of HSPs from the optic nerve due to side effects including chemical and physical side effects. A novel nanomedicine modality has now been shown to be feasible for ocular neuroprotection in glaucoma cases.
Oct 25th, 2010
 Imagine intelligent medical implants that can continuously monitor their condition inside the body and autonomously respond to changes such as infection by releasing anti-inflammatory agents. Thanks to nanotechnology, medical research is moving quickly towards this goal. A new study shows that the use of polypyrrole films as electrically controlled drug release devices on implant surfaces can potentially improve bone implants. By electrodepositing antibiotics or anti-inflammatory drugs in a polymer coating on medical devices, researchers demonstrate that such drugs can be released from polypyrrole on demand - by applying a voltage - and control cellular behavior important for orthopedic applications, i.e. inhibit inflammation and kill bacteria.
Imagine intelligent medical implants that can continuously monitor their condition inside the body and autonomously respond to changes such as infection by releasing anti-inflammatory agents. Thanks to nanotechnology, medical research is moving quickly towards this goal. A new study shows that the use of polypyrrole films as electrically controlled drug release devices on implant surfaces can potentially improve bone implants. By electrodepositing antibiotics or anti-inflammatory drugs in a polymer coating on medical devices, researchers demonstrate that such drugs can be released from polypyrrole on demand - by applying a voltage - and control cellular behavior important for orthopedic applications, i.e. inhibit inflammation and kill bacteria.
 Subscribe to our Nanotechnology Spotlight feed
Subscribe to our Nanotechnology Spotlight feed





