Showing Spotlights 273 - 280 of 544 in category All (newest first):
 Nanotechnology is finding applications in the treatment of infectious and inflammatory diseases, particularly skin disease. These applications work in one of two ways: utilizing nanomaterials that have inherent antimicrobial properties; or incorporating known therapeutics into nanoscale vehicles to enhance delivery and improve efficacy. An ideal approach to develop a topical therapy for microbial infection in skin would combine both. Now, researchers have developed a new nanoparticle platform using chitosan for the treatment of inflammatory skin diseases such as Acne Vulgaris.
Nanotechnology is finding applications in the treatment of infectious and inflammatory diseases, particularly skin disease. These applications work in one of two ways: utilizing nanomaterials that have inherent antimicrobial properties; or incorporating known therapeutics into nanoscale vehicles to enhance delivery and improve efficacy. An ideal approach to develop a topical therapy for microbial infection in skin would combine both. Now, researchers have developed a new nanoparticle platform using chitosan for the treatment of inflammatory skin diseases such as Acne Vulgaris.
Jan 3rd, 2013
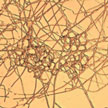 Naturally occurring nanomaterials can be found everywhere in nature - in soil, ground and surface waters, volcanic ash, ocean spray, mineral composites, smoke. Biogenic magnetite nanoparticles have even been discovered in various organisms, ranging from bacteria to human brains, with various biological functions. Researchers have discovered that nanoparticles produced by a flesh-eating fungus hold promise for stimulating the immune system and killing tumors.
Naturally occurring nanomaterials can be found everywhere in nature - in soil, ground and surface waters, volcanic ash, ocean spray, mineral composites, smoke. Biogenic magnetite nanoparticles have even been discovered in various organisms, ranging from bacteria to human brains, with various biological functions. Researchers have discovered that nanoparticles produced by a flesh-eating fungus hold promise for stimulating the immune system and killing tumors.
Dec 18th, 2012
 Nanotechnology-enabled bio-pharmaceuticals are the most innovative and highly specialized alternative medicines for curing chronic diseases. These functionally modified nanomaterials help in early detection of chronic diseases. In addition to this, they also detect the microorganisms and viruses associated with infections. In this article, the authors analyze the immense potential of nanotechnology in India's pharmaceutical and biotechnology industries.
Nanotechnology-enabled bio-pharmaceuticals are the most innovative and highly specialized alternative medicines for curing chronic diseases. These functionally modified nanomaterials help in early detection of chronic diseases. In addition to this, they also detect the microorganisms and viruses associated with infections. In this article, the authors analyze the immense potential of nanotechnology in India's pharmaceutical and biotechnology industries.
Dec 13th, 2012
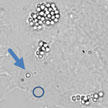 Researchers are very interested in investigating the biomechanical properties of the inner structure of cells due to their relevance in many important topics in biology such as intracellular and intercellular dynamics; tissue and organs formation and their homeostasis; but also in medicine as the formation and development of diseases like inflammatory disorders or tumor. In order to study inner cell properties, researchers have now presented a biophotonic holographic workstation that combines the complementary features of holographic optical tweezers (HOT) and self-interference digital holographic microscopy, in order to investigate biomechanics properties at the single cell level.
Researchers are very interested in investigating the biomechanical properties of the inner structure of cells due to their relevance in many important topics in biology such as intracellular and intercellular dynamics; tissue and organs formation and their homeostasis; but also in medicine as the formation and development of diseases like inflammatory disorders or tumor. In order to study inner cell properties, researchers have now presented a biophotonic holographic workstation that combines the complementary features of holographic optical tweezers (HOT) and self-interference digital holographic microscopy, in order to investigate biomechanics properties at the single cell level.
Dec 7th, 2012
 The subventricular zone (SVZ) is a region in the mammalian brain where self-renewing and multipotent neural stem cells give rise to new brain cells such as neurons, astrocytes, and oligodendrocytes. Neuroscientists and cell biologists are keen to use nanotechnologies to manipulate endogenous stem cell niches such as the SVZ. New work describes the first example in the manipulation of the neural stem cell niche by the use of nanoparticles releasing a pro-neurogenic agent - retinoic acid.
The subventricular zone (SVZ) is a region in the mammalian brain where self-renewing and multipotent neural stem cells give rise to new brain cells such as neurons, astrocytes, and oligodendrocytes. Neuroscientists and cell biologists are keen to use nanotechnologies to manipulate endogenous stem cell niches such as the SVZ. New work describes the first example in the manipulation of the neural stem cell niche by the use of nanoparticles releasing a pro-neurogenic agent - retinoic acid.
Dec 6th, 2012
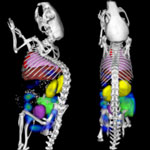 One of the key issues in the development of novel nanomedicines is the ability to track nanoscale drug carriers inside the body to evaluate where they go and how they get there. Virtually all previous preclinical studies in this area of research rely on 2D Fluorescence Reflectance Imaging (FRI). Given the limitation of 2D FRI in not being able to detect the fluorescence in deep-seated organs and tissues, 3D Fluorescence Molecular Tomography (3D FMT) emerged as an alternative. However, the lack of anatomical information was an important barrier hindering the routine use of standard 3D FMT for in vivo imaging of nanomedicines. Researchers have now developed a hybrid CT-FMT-based imaging protocol to enable more meaningful and more quantitative in vivo analyses.
One of the key issues in the development of novel nanomedicines is the ability to track nanoscale drug carriers inside the body to evaluate where they go and how they get there. Virtually all previous preclinical studies in this area of research rely on 2D Fluorescence Reflectance Imaging (FRI). Given the limitation of 2D FRI in not being able to detect the fluorescence in deep-seated organs and tissues, 3D Fluorescence Molecular Tomography (3D FMT) emerged as an alternative. However, the lack of anatomical information was an important barrier hindering the routine use of standard 3D FMT for in vivo imaging of nanomedicines. Researchers have now developed a hybrid CT-FMT-based imaging protocol to enable more meaningful and more quantitative in vivo analyses.
Nov 13th, 2012
 When a nanomaterial enters a biological environment, it comes into contact with a complex mixture of proteins. Some of these proteins can adhere to the surface of the nanomaterial, forming a protein 'corona' that influences its subsequent biological interactions. While a number of studies have characterized the protein corona formed around nanomaterials with diameters greater than 10nm, until now, lack of a suitable separation technique has prevented researchers from studying the protein corona formed around 'ultrasmall' nanomaterials. A team of European researchers used electrophoresis to separate ultrasmall nanomaterials from free protein. Applying this technique, they discovered that ultrasmall nanomaterials interact with proteins in a way that is fundamentally different from larger nanomaterials with analogous composition.
When a nanomaterial enters a biological environment, it comes into contact with a complex mixture of proteins. Some of these proteins can adhere to the surface of the nanomaterial, forming a protein 'corona' that influences its subsequent biological interactions. While a number of studies have characterized the protein corona formed around nanomaterials with diameters greater than 10nm, until now, lack of a suitable separation technique has prevented researchers from studying the protein corona formed around 'ultrasmall' nanomaterials. A team of European researchers used electrophoresis to separate ultrasmall nanomaterials from free protein. Applying this technique, they discovered that ultrasmall nanomaterials interact with proteins in a way that is fundamentally different from larger nanomaterials with analogous composition.
Nov 2nd, 2012
 The ideal drug carrier may be something out of science fiction. In principle, it is injected into the body and transports itself to the correct target, such as a tumor, and delivers the required dose at this target. This idealized concept was first proposed by Paul Ehrlich at the beginning of the 20th century and was nicknamed the 'magic bullet' concept. With the advent of nanotechnology and nanomedicine this dream is rapidly becoming a reality. Researchers have already demonstrated that unctionalized carbon nanotubes (CNTs) might be able to target specific cells, become ingested, and then release their contents in response to a chemical trigger. A group of researchers has now essentially achieved this goal. They have encapsulated drugs inside carbon nanotubes for drug delivery and shown that these drugs can be released 'on command' by inductive heating with an external alternating current or pulsed magnetic field.
The ideal drug carrier may be something out of science fiction. In principle, it is injected into the body and transports itself to the correct target, such as a tumor, and delivers the required dose at this target. This idealized concept was first proposed by Paul Ehrlich at the beginning of the 20th century and was nicknamed the 'magic bullet' concept. With the advent of nanotechnology and nanomedicine this dream is rapidly becoming a reality. Researchers have already demonstrated that unctionalized carbon nanotubes (CNTs) might be able to target specific cells, become ingested, and then release their contents in response to a chemical trigger. A group of researchers has now essentially achieved this goal. They have encapsulated drugs inside carbon nanotubes for drug delivery and shown that these drugs can be released 'on command' by inductive heating with an external alternating current or pulsed magnetic field.
Oct 30th, 2012
 Nanotechnology is finding applications in the treatment of infectious and inflammatory diseases, particularly skin disease. These applications work in one of two ways: utilizing nanomaterials that have inherent antimicrobial properties; or incorporating known therapeutics into nanoscale vehicles to enhance delivery and improve efficacy. An ideal approach to develop a topical therapy for microbial infection in skin would combine both. Now, researchers have developed a new nanoparticle platform using chitosan for the treatment of inflammatory skin diseases such as Acne Vulgaris.
Nanotechnology is finding applications in the treatment of infectious and inflammatory diseases, particularly skin disease. These applications work in one of two ways: utilizing nanomaterials that have inherent antimicrobial properties; or incorporating known therapeutics into nanoscale vehicles to enhance delivery and improve efficacy. An ideal approach to develop a topical therapy for microbial infection in skin would combine both. Now, researchers have developed a new nanoparticle platform using chitosan for the treatment of inflammatory skin diseases such as Acne Vulgaris.
 Subscribe to our Nanotechnology Spotlight feed
Subscribe to our Nanotechnology Spotlight feed





