| Posted: Oct 25, 2010 | |
A nanomedicine approach for ocular neuroprotection in glaucoma |
|
| (Nanowerk Spotlight) Glaucoma is an eye disease in which the optic nerve is damaged, leading to progressive and irreversible loss of vision. It is often, but not always, associated with increased pressure of the fluid in the eye. In the early stages of the disease, there may be no symptoms. Depending upon the type of glaucoma, treatment may include medication, usually prescription eyedrops, or surgery to lower the pressure in the eye and prevent further damage to the optic nerve. While there is no cure as yet for glaucoma, early diagnosis and continuing treatment can preserve eyesight. | |
| Medical researchers believe that the best way to protect the eye from glaucoma is to protect the optic nerve from a sudden increase in intraocular pressure since ocular hypertension is the most important risk factor for glaucoma. | |
| Accordingly, for the past few years, huge research efforts have been made to develop a powerful biotechnical approach to protect the optic nerve. As a result, scientists discovered that Heat Shock Proteins (HSPs) can be a new powerful modality for the protection of optic nerves – ocular neuroprotection – from glaucoma. | |
| "The HSPs, called by stress proteins, are a group of proteins that exist in all living creatures, from bacteria to human beings," Seongtae Bae explains to Nanowerk. "They can be induced in living cells by hyperthermia, metabolic stress, or oxygen deprivation. In particular, HSPs 70 families in the mammalian central nervous system have been known to enhance neuronal tolerance against ischemic insults and confirmed to be effective for neuroprotection against light-induced injuries in a rat retina." | |
| Although a variety of methods to induce HSPs have been developed and tried, they all were found to be ineffective for the induction of HSPs from the optic nerve due to side effects including chemical and physical side effects. | |
| A novel nanomedicine modality has now been shown to be feasible for ocular neuroprotection in glaucoma cases. | |
| Bae, an assistant professor and supervisor of the Biomagnetics Laboratory (BML) at the Department of Electrical and Computer Engineering at National University of Singapore, and his team, together with a medical research collaborator team from Seoul National University (SNU), led by Ki Ho Park, a professor in the Department of Ophthalmology at SNU's School of Medicine have developed an approach that induces localized HSPs by local magnetic hyperthermia using engineered superparamagnetic nanoparticle agents with a 5.5 nm mean particle size. | |
 |
|
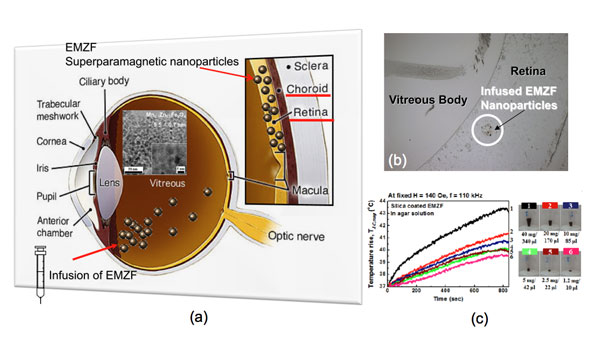
| (a) A schematic diagram of newly developed infusion method of engineered Mn0.5Zn0.5Fe2O4 (EMZF) nanoparticles to the retina, (b) image of infused EMZF nanoparticles in the retina, and (c) successful demonstration of AC magnetically-induced heating characteristics of 5.5 nm EMZF@silica for localized heat shock proteins (HSPs) in an agar solution with the same viscosity of cytoplasm (retinal ganglion cells). (Image: Prof. Seongtae Bae, National University of Singapore) | |
| Reporting their findings in the September 28, 2010, online issue of Biomaterials ("Engineered superparamagnetic Mn0.5Zn0.5Fe2O4 nanoparticles as a heat shock protein induction agent for ocular neuroprotection in glaucoma"), the team summarizes their scientific findings in three main areas. Says Bae: | |
| 1) "We developed a new infusion technique of nanoparticles to the retina through the vitreous body (most of the current technology regarding infusions is through intravenous injection through blood vessels; but the eye does not have any blood vessel except for Choroid so we developed a new technique through the vitreous body). Here, the nanoparticles are injected into the eyeball and are diffused through the vitreous body to the surface of the retina; | |
| 2) "We developed a very small size of nanoparticle with 5.5 nm mean diameter, which exhibited a higher SAR (specific absorption rate) as well as higher heat generation in a short time and can be easily transported in the eye by developing a new synthesis method (for more on this, see "Effects of Mn concentration on the ac magnetically induced heating characteristics of superparamagnetic MnxZn1-xFe2O4 nanoparticles for hyperthermia"); and | |
| 3) "Successful demonstration of heating temperature in a retinal ganglion cell (in vitro) for successful HSPs (in the range of 39-41°C) particularly in the biologically and physiologically safe range of AC magnetic field and frequency." | |
| Bae points out that all the experimental results shown in the team's study strongly suggest that the ocular neuroprotection based on the HSPs induction by local magnetic hyperthermia using silica coated superparamagnetic nanoparticle agents can be an innovative approach for the efficacious treatment of glaucoma. | |
| Currently, though, the technique needs to be improved before it can be realized in clinical trials. The researchers found that the total number of infused nanoparticles is not enough yet to induce an effective amount of HSPs and the total diffusion time is too long. | |
| "This is the critical challenge we need to overcome" says Bae. "However, in order to solve this problem, very recently we have designed new infusion equipment. According to the initial experimental results, it can be successfully used for solving our problem. We are currently working on optimizing the technique." | |
| Bae and his collaborators are confident that, once the developed modality is completely verified to be successful in clinical trials, this nanobiotechnology application can be extended to treating other neural disease such as Parkinson's disease, Alzheimer's, epilepsy, and other bioelectric transmitting related diseases. In addition, it could be considered for use in a variety of immunology related diseases. | |
| "Each organ and each cell in the human body has different physiological, biological and chemical properties" says Bae, "so in order to further develop this modality for personalized medicine, and personal healthcare targeted for different types of incurable diseases, we need more efforts with regard to improving nanoparticle functionality and enhancing nanoparticle surface properties for high uptake in the cells, successful circulating in the blood, and easy excretion." | |
 By
Michael
Berger
– Michael is author of three books by the Royal Society of Chemistry:
Nano-Society: Pushing the Boundaries of Technology,
Nanotechnology: The Future is Tiny, and
Nanoengineering: The Skills and Tools Making Technology Invisible
Copyright ©
Nanowerk LLC
By
Michael
Berger
– Michael is author of three books by the Royal Society of Chemistry:
Nano-Society: Pushing the Boundaries of Technology,
Nanotechnology: The Future is Tiny, and
Nanoengineering: The Skills and Tools Making Technology Invisible
Copyright ©
Nanowerk LLC
|
|
| Reference: Jeun, M., Jeoung, J., Moon, S., Kim, Y., Lee, S., Paek, S., Chung, K., Park, K., & Bae, S. (2010). Engineered superparamagnetic Mn0.5Zn0.5Fe2O4 nanoparticles as a heat shock protein induction agent for ocular neuroprotection in glaucoma Biomaterials DOI: 10.1016/j.biomaterials.2010.09.016 | |
|
Become a Spotlight guest author! Join our large and growing group of guest contributors. Have you just published a scientific paper or have other exciting developments to share with the nanotechnology community? Here is how to publish on nanowerk.com. |
|
