| Posted: Jul 19, 2017 | |
Capitalizing on nanotechnology to address fungal infections topically |
|
| (Nanowerk Spotlight) Cutaneous fungal infections involving the skin, hair, or nails affect an estimated 25% of the world's population, and accounts for millions of outpatient visits yearly in the United States alone. | |
| While often limited to the superficial layers of the skin, these skin loving fungi can invade into the dermis and subcutaneous tissue, especially following trauma or in the setting of immunosuppression. | |
| Currently, deep fungal infection require systemic therapy, which can pose a range of side effects or drug interactions depending on the clinical scenario. | |
| In a new study (Nanomedicine: Nanotechnology, Biology, and Medicine, "Topical nitric oxide releasing nanoparticles are effective in a murine model of dermal Trichophyton rubrum dermatophytosis"), conducted at George Washington School of Medicine and Health Sciences and the Albert Einstein College of Medicine, investigators both demonstrated the antifungal activity of nitric oxide generating nanoparticles against dermatophytes well known to cause invasive cutaneous infections, and highlighted the utility and superiority of this platform in a mouse model of Majocchi granuloma, deep fungal infection caused by trichophyton rubrum, as compared to topical terbinafine. | |
| "Here nanotechnology is not only providing a vehicle through which we can deliver the highly reactive and biologically potent gaseous molecule nitric oxide, but also overcoming physical barriers to reach targets previously unattainable with conventional methods," Dr. Adam Friedman, Associate Professor of Dermatology and Director of Translational Research at GW, who led the study, tells Nanowerk. | |
 |
|
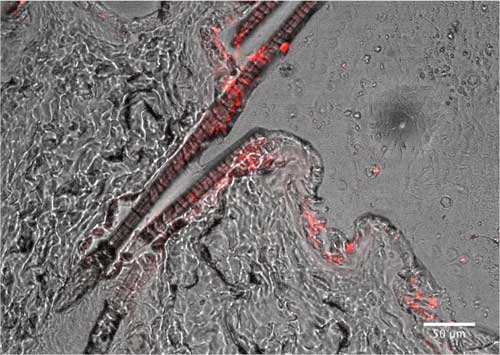
| Fluorescent labeled nanoparticles penetrate the epidermis and follicular unit on rat abdominal skin. (Image: Dr. Adam Friedman) (click on image to enlarge) | |
| Nitric oxide (NO), a gaseous immunomodulator with broad-spectrum, multi-mechanistic antimicrobial activity, is an attractive agent for a topical antifungal. Although NO is ubiquitous throughout the body, therapeutic delivery is challenging due to its short half-life and high reactivity. This can be overcome by a nanoparticle platform that generates and releases NO over time. | |
| In previous Nanowerk Spotlights we reported on Friedman's work with nitric oxide releasing nanoparticles for effective treatment of infections; their promise as as wound healing agent; even as a nanotechnology alternative to Viagra. | |
| Through this new work, the researchers gained a better understanding of the susceptibility of clinically relevant dermatophyte strains to nitric oxide, the practicality of utilizing nanotechnology to reach deeper pathology, and highlights the utility of this moms model as a tool to study deep dermatophytosis. | |
 |
|
| Nitric oxide nanoparticles (10mg/ml) disrupt hyphal cell wall integrity and induce complete cell disruption of hyphal structures based on TEM cross-sections. (Image: Dr. Adam Friedman) (click on image to enlarge) | |
| "The motivation for this work followed a similar path to our exploration of this platform in treating bacterial skin infections of various depths," says Friedman. "We demonstrated efficacy in superficial MRSA wounds, then moved to intradermal/subcutaneous abscesses, and pushed the envelope going after intramusaular MRSA abscesses and comparing to the gold standard, intravenous vancomycin. Here too, we had previously demonstrated success with superficial cutaneous mycoses, both dermatophytes and candida albicans, so we wanted to delve deeper yet again." | |
| "Why work with nanotechnology if you are not going to push past the frontiers of current medical practice?" he pointedly asks. | |
| Given the plethora of pre-clinical data generated on this platform, the team's plan is to move towards Phase 1 studies once nanoparticle scale up is completed. | |
| "There are numerous applications supported both by our pre-clinical data, such as skin and soft tissues infections, wound healing, Acne Vulgaris, and erectile dysfunction to name a few," Friedman notes. "No question, capitalizing on nanotechnology to address a disease state topically when this was not possible in the past is certainly a priority." | |
 By
Michael
Berger
– Michael is author of three books by the Royal Society of Chemistry:
Nano-Society: Pushing the Boundaries of Technology,
Nanotechnology: The Future is Tiny, and
Nanoengineering: The Skills and Tools Making Technology Invisible
Copyright ©
Nanowerk LLC
By
Michael
Berger
– Michael is author of three books by the Royal Society of Chemistry:
Nano-Society: Pushing the Boundaries of Technology,
Nanotechnology: The Future is Tiny, and
Nanoengineering: The Skills and Tools Making Technology Invisible
Copyright ©
Nanowerk LLC
|
|
|
Become a Spotlight guest author! Join our large and growing group of guest contributors. Have you just published a scientific paper or have other exciting developments to share with the nanotechnology community? Here is how to publish on nanowerk.com. |
|
