Showing Spotlights 345 - 352 of 546 in category All (newest first):
 A multi-disciplinary research team has introduced a novel label-free optofluidic-nanoplasmonic biosensor and demonstrated direct detection of live viruses from biological media at medically relevant concentrations with little to no sample preparation. This novel platform can be easily adapted for point-of-care diagnostics to detect a broad range of viral pathogens in resource-limited clinical settings at the far corners of the world, in defense and homeland security applications as well as in civilian settings such as airports or other public spaces. This work is the first demonstration of detection of intact viruses using extraordinary light transmission phenomena in plasmonic nanohole arrays.
A multi-disciplinary research team has introduced a novel label-free optofluidic-nanoplasmonic biosensor and demonstrated direct detection of live viruses from biological media at medically relevant concentrations with little to no sample preparation. This novel platform can be easily adapted for point-of-care diagnostics to detect a broad range of viral pathogens in resource-limited clinical settings at the far corners of the world, in defense and homeland security applications as well as in civilian settings such as airports or other public spaces. This work is the first demonstration of detection of intact viruses using extraordinary light transmission phenomena in plasmonic nanohole arrays.
Nov 17th, 2010
 Medical researchers believe that the best way to protect eye from glaucoma is to protect the optic nerve from a sudden increase in intraocular pressure since ocular hypertension is the most important risk factor for glaucoma. Accordingly, for the past few years, huge research efforts have been made to develop a powerful biotechnical approach to protect the optic nerve. As a result, scientists discovered that Heat Shock Proteins (HSPs) can be a new powerful modality for the protection of optic nerves - ocular neuroprotection - from glaucoma. Although a variety of methods to induce HSPs have been developed and tried, they all were found to be ineffective for the induction of HSPs from the optic nerve due to side effects including chemical and physical side effects. A novel nanomedicine modality has now been shown to be feasible for ocular neuroprotection in glaucoma cases.
Medical researchers believe that the best way to protect eye from glaucoma is to protect the optic nerve from a sudden increase in intraocular pressure since ocular hypertension is the most important risk factor for glaucoma. Accordingly, for the past few years, huge research efforts have been made to develop a powerful biotechnical approach to protect the optic nerve. As a result, scientists discovered that Heat Shock Proteins (HSPs) can be a new powerful modality for the protection of optic nerves - ocular neuroprotection - from glaucoma. Although a variety of methods to induce HSPs have been developed and tried, they all were found to be ineffective for the induction of HSPs from the optic nerve due to side effects including chemical and physical side effects. A novel nanomedicine modality has now been shown to be feasible for ocular neuroprotection in glaucoma cases.
Oct 25th, 2010
 Gold-based nanostructures and carbon nanotubes have been successfully applied for photoacoustic imaging and photothermal treatment of tumors. Medical researchers believe that such nanoparticle-mediated, image-guided cancer therapy has tremendous promise for increasing the efficacy of cancer treatment while reducing toxic side effects traditionally associated with treatment. Working with a different carbon nanomaterial, researchers now have been able to show that polyhydroxy fullerenes can be utilized for the same purposes. The minute size and biocompatibility of polyhydroxy fullerenes make them particularly attractive for biomedical applications - they are water-soluble, biodegradable, antioxidant, and rapidly excreted.
Gold-based nanostructures and carbon nanotubes have been successfully applied for photoacoustic imaging and photothermal treatment of tumors. Medical researchers believe that such nanoparticle-mediated, image-guided cancer therapy has tremendous promise for increasing the efficacy of cancer treatment while reducing toxic side effects traditionally associated with treatment. Working with a different carbon nanomaterial, researchers now have been able to show that polyhydroxy fullerenes can be utilized for the same purposes. The minute size and biocompatibility of polyhydroxy fullerenes make them particularly attractive for biomedical applications - they are water-soluble, biodegradable, antioxidant, and rapidly excreted.
Sep 29th, 2010
 Studies of the interface between nanostructures and live cells have been increasing rapidly in the past few years. Because the size of nanostructures is often comparable to internal organelles inside the cell, those nanostructures are very useful in serving as sensors to detect biological events inside a live cell. For neuroscientists, monitoring the electrical signaling within neural networks is a fundamental issue. It has proven to be very challenging to monitoring individual neuron activities in a neuronal network for an extended time, which demands stable and specific neuron-electrode correspondence. Unfortunately for the scientists, neurons tend to migrate as far as hundreds of micrometers. With a new techniques, researchers have managed to engineer unique nanostructures that foster, rather than impose, residence of neuron cell bodies atop the electrode of interest.
Studies of the interface between nanostructures and live cells have been increasing rapidly in the past few years. Because the size of nanostructures is often comparable to internal organelles inside the cell, those nanostructures are very useful in serving as sensors to detect biological events inside a live cell. For neuroscientists, monitoring the electrical signaling within neural networks is a fundamental issue. It has proven to be very challenging to monitoring individual neuron activities in a neuronal network for an extended time, which demands stable and specific neuron-electrode correspondence. Unfortunately for the scientists, neurons tend to migrate as far as hundreds of micrometers. With a new techniques, researchers have managed to engineer unique nanostructures that foster, rather than impose, residence of neuron cell bodies atop the electrode of interest.
Sep 16th, 2010
 Current protein detection approaches are mainly dominated by heterogeneous immunological (or separation) assay methods. These assays are usually low-throughput and frequently require multiple steps including multiple incubation and careful washing of a surface onto which the labeled reagent has bound. In contrast, homogenous immunoassays can overcome these problems. In these assays, the signal is affected by binding and can often be run without a separation step. Such assays can frequently be carried out simply by mixing the reagents and sample and making a physical measurement. Researchers in China and Japan have now developed a graphene oxide based fluorescence assay for fast, ultra-sensitive, and selective detection of protein and demonstrated its use for detection of a prognostic indicator in early-stage cancer, cyclin A2.
Current protein detection approaches are mainly dominated by heterogeneous immunological (or separation) assay methods. These assays are usually low-throughput and frequently require multiple steps including multiple incubation and careful washing of a surface onto which the labeled reagent has bound. In contrast, homogenous immunoassays can overcome these problems. In these assays, the signal is affected by binding and can often be run without a separation step. Such assays can frequently be carried out simply by mixing the reagents and sample and making a physical measurement. Researchers in China and Japan have now developed a graphene oxide based fluorescence assay for fast, ultra-sensitive, and selective detection of protein and demonstrated its use for detection of a prognostic indicator in early-stage cancer, cyclin A2.
Sep 13th, 2010
 Australian researchers have introduced the Nanopatch - a new way of delivering vaccines to the skin and potentially a safer, cheaper alternative to traditional needle vaccines. The Nanopatch comprises arrays of densely packed projections with a defined geometry and distribution designed to physically target vaccines directly to thousands of epidermal and dermal antigen presenting cells. These miniaturized arrays are two orders of magnitude smaller than standard needles and are also much smaller than current microneedle arrays. The core idea is to achieve improved vaccine efficiency and effectiveness - over the needle and syringe - through precise targeting of vaccines to skin strata, achieved by device miniaturization utilizing micro- and nanotechnologies.
Australian researchers have introduced the Nanopatch - a new way of delivering vaccines to the skin and potentially a safer, cheaper alternative to traditional needle vaccines. The Nanopatch comprises arrays of densely packed projections with a defined geometry and distribution designed to physically target vaccines directly to thousands of epidermal and dermal antigen presenting cells. These miniaturized arrays are two orders of magnitude smaller than standard needles and are also much smaller than current microneedle arrays. The core idea is to achieve improved vaccine efficiency and effectiveness - over the needle and syringe - through precise targeting of vaccines to skin strata, achieved by device miniaturization utilizing micro- and nanotechnologies.
Aug 31st, 2010
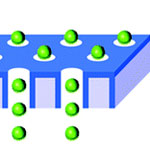 Delivering healthy proteins directly into human cells to replace malfunctioning proteins is considered one of the most direct and safe approaches for treating diseases. Controlled and long-term protein drug delivery has also been considered as one of the most promising biomedical applications of nanotechnology. So far, though, the effectiveness of protein therapy has been limited by low delivery efficiency and the poor stability of proteins, which are frequently broken down and digested by cells' protease enzymes before they reach their intended target. This not only makes the drugs ineffective, it can also cause unpredictable side effects such as inflammation, toxicity, and immune responses. The best way for the delivery of protein drugs without denaturation might be possible by exploiting the passive diffusion through a membrane without physical and chemical stresses. This can be achieved when pore sizes in a membrane are controlled to satisfy the single-file diffusion condition of protein drugs.
Delivering healthy proteins directly into human cells to replace malfunctioning proteins is considered one of the most direct and safe approaches for treating diseases. Controlled and long-term protein drug delivery has also been considered as one of the most promising biomedical applications of nanotechnology. So far, though, the effectiveness of protein therapy has been limited by low delivery efficiency and the poor stability of proteins, which are frequently broken down and digested by cells' protease enzymes before they reach their intended target. This not only makes the drugs ineffective, it can also cause unpredictable side effects such as inflammation, toxicity, and immune responses. The best way for the delivery of protein drugs without denaturation might be possible by exploiting the passive diffusion through a membrane without physical and chemical stresses. This can be achieved when pore sizes in a membrane are controlled to satisfy the single-file diffusion condition of protein drugs.
Aug 10th, 2010
 With fully conclusive findings about the toxicity of carbon nanotubes (CNTs) still up in the air, research on biomedical applications of CNTs is pushing full steam ahead. Adding to the list of potential concerns, a recent nanotoxicology study by a U.S.-Chinese research team looked into the impact of carbon nanotubes on male reproductive health. The translocation and biodistribution of nanoparticles are key factors in their toxicity evaluation in vivo. Although other nanoparticles such as gold and magnetic nanoparticles have been reported to enter testes in small quantities, it had not been established whether CNTs could enter or accumulate in the testis. This pilot study investigated the effects of intravenous injection of single and multiple doses of water-soluble multiwalled carbon nanotubes on the reproductive systems of male mice.
With fully conclusive findings about the toxicity of carbon nanotubes (CNTs) still up in the air, research on biomedical applications of CNTs is pushing full steam ahead. Adding to the list of potential concerns, a recent nanotoxicology study by a U.S.-Chinese research team looked into the impact of carbon nanotubes on male reproductive health. The translocation and biodistribution of nanoparticles are key factors in their toxicity evaluation in vivo. Although other nanoparticles such as gold and magnetic nanoparticles have been reported to enter testes in small quantities, it had not been established whether CNTs could enter or accumulate in the testis. This pilot study investigated the effects of intravenous injection of single and multiple doses of water-soluble multiwalled carbon nanotubes on the reproductive systems of male mice.
Aug 9th, 2010
 A multi-disciplinary research team has introduced a novel label-free optofluidic-nanoplasmonic biosensor and demonstrated direct detection of live viruses from biological media at medically relevant concentrations with little to no sample preparation. This novel platform can be easily adapted for point-of-care diagnostics to detect a broad range of viral pathogens in resource-limited clinical settings at the far corners of the world, in defense and homeland security applications as well as in civilian settings such as airports or other public spaces. This work is the first demonstration of detection of intact viruses using extraordinary light transmission phenomena in plasmonic nanohole arrays.
A multi-disciplinary research team has introduced a novel label-free optofluidic-nanoplasmonic biosensor and demonstrated direct detection of live viruses from biological media at medically relevant concentrations with little to no sample preparation. This novel platform can be easily adapted for point-of-care diagnostics to detect a broad range of viral pathogens in resource-limited clinical settings at the far corners of the world, in defense and homeland security applications as well as in civilian settings such as airports or other public spaces. This work is the first demonstration of detection of intact viruses using extraordinary light transmission phenomena in plasmonic nanohole arrays.
 Subscribe to our Nanotechnology Spotlight feed
Subscribe to our Nanotechnology Spotlight feed





